
The nose is a central and prominent structure of the face. A deformity of the nose can significantly alter ones facial appearance or result in nasal complaints. Nasal deformity can be categorized as “cosmetic” or “functional.” Cosmetic deformity of the nose results in a less desirable appearance of the nose. A functional deformity of the nose may result in frustrating nasal blockage, noisy breathing or snoring, decreased smell or taste, nose bleeds and/or recurrent sinusitis. There are multiple etiologies, and often, many of the causes result in both cosmetic and functional problems.
DIFFERENT CAUSES OF COSMETIC AND FUNCTIONAL PROBLEMS
Congenital deformity
A baby born with nasal mass or other anomaly may have structural weakness or asymmetry of the nose.
Nasal trauma
Injury to the nose can result in a septal hematoma (a collection of blood between the lining of the nose and the nasal septum), septal fracture and deviation, or nasal bone fracture. A fracture can result in shifting of nasal structures leading to nasal obstruction and cosmetic changes.
Prior nasal surgery
Patients who have undergone previous nasal surgery may experience weakening or collapse in their support structures.
Nasal mass
An external or internal nasal mass can change the shape or alter the function of the nose.
Age related changes
As patients age, they may experience weakening or collapse of nasal structures.
Medical conditions
Certain nasal and systemic (affect the entire body) medical conditions may cause structural changes of the nose. Common conditions affecting nasal appearance and function include: Sarcoidosis, Wegner’s Disease, Relapsing Polychondritis and other connective tissue disorders.
Nasal septum
The nasal septum is the separation between the two nostrils. In adults, it is composed of both cartilage and bone. The nasal septum has three functions: support the nose, regulate air flow, and support the mucous membranes of the nose.
A deviated septum is a common condition that involves a displacement of the septum, the wall that separates the nostrils, to one side of the nose. The septum is usually straight at birth, but may bend to one side or the other as the patient ages. Trauma can also affect the deviation of the septum, but many patients experiencing symptoms from this condition have no history of injury.

Deviated septum makes one nasal passage smaller than the other, which can affect breathing if the displacement is great enough. Patients with a severe deviated septum may experience nasal congestion, nosebleeds and frequent or recurring sinus infections as a result of their uneven nasal passages. Those with only minor displacement may not even be aware that they have a deviated septum and experience no symptoms.
- Nasal Turbinate Hypertrophy
- The turbinates are structures on the side wall of the inside of the nose. They project into the nasal passages as ridges of tissue.
There are three types of turbinates:- Inferior nasal turbinates- these, being the largest of all nasal turbinates aids in the direction of the airflow, heating, humidification as well as the filtration of the air that is inhaled via the nose.
- Middle nasal turbinates- these are smaller than inferior turbinates. They are responsible for protection of the nasal sinuses from directly being exposed to the airflow that is pressurized.
- Superior nasal turbinates- these are even smaller than the middle nasal turbinates. They have nerve endings linking them to middle nasal turbinates. They are responsible for protection of olfactory bulb.
The turbinates are made of bone and soft tissue. Either the bone or the soft tissue can become enlarged. In most patients, enlargement of the soft tissue part of the turbinate is the major problem when the turbinates become swollen. When the turbinates are large, they are called hypertrophic turbinates.
The inferior turbinates are typically more involved in routine nasal breathing and more often evaluated in conjunction with the septum.
Hypertrophied nasal turbinate symptoms include nasal congestion, nose bleeding, snoring, sinus infections etc.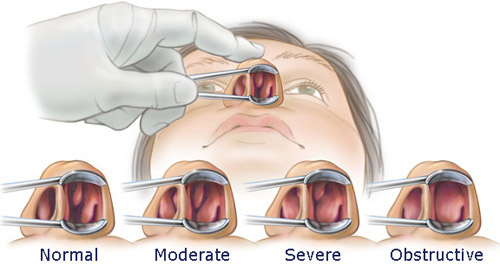
NASAL FUNCTIONAL SURGERIES THAT CAN BE DONE DURING COSMETIC NOSE SURGERY
Septorhinoplasty
Septorhinoplasty is a combination of Rhinoplasty and Septoplasty surgeries. Rhinoplasty is performed for cosmetic or functional reasons to reshape the nose – while Septoplasty corrects a deviated septum to restore (or create) normal breathing function.
Nose surgery is done for either cosmetic or functional reasons. Septorhinoplasty is performed for both reasons – to reshape the nose so it is cosmetically more pleasing and in balance with the rest of the face and for functional purposes to improve breathing by correcting a septum that became deviated through injury, trauma, disease or sometimes a previous surgery.
Benefits of Septorhinoplasty
- Septorhinoplasty can improve the appearance of a crooked nose
- Septorhinoplasty relieves nasal blockages to improve breathing
- Septorhinoplasty corrects the bent/deviated septum – thus improving shape
- Septorhinoplasty can improve snoring and sleep apnea
- Septorhinoplasty changes the shape of the nose and creates balance with other facial features
- Septorhinoplasty achieves both cosmetic and functional improvements
What does the operation involve?
A septorhinoplasty is almost always performed under a general anaesthetic. The operation usually takes between one and two hours.
Your surgeon will make a cut in the mucosa (the skin-like lining inside the nose) and lift it off the cartilage and bone. They will remove the parts of the cartilage and bone that are bent and they will put the rest back in a straight position.
Your surgeon can refine the tip of your nose by reducing the cartilage. If you have a hump (dorsum) on your nose, they will shave it down. Your surgeon can also straighten and narrow the nasal bones by breaking and then setting them (infracture). Your surgeon may need to support or rebuild part of your nose.

Turbinate Reduction
There are many ways to shrink the size of the turbinates. Surgery is typically called turbinate reduction or turbinate resection. In many instances, turbinate surgery is performed in conjunction with septoplasty. It is important that the turbinate not be removed completely because its removal can result in a very dry and crusty nose. In the absence of a turbinate, the air that is breathed may not be to adequately humidified and warmed.
Some methods rely on shrinking the turbinates without removing any of the turbinate bone or tissue. These methods include cauterization, coblation, and radiofrequency reduction. In each of these methods, a portion of the turbinate is heated up with a special device. Over time, scar tissue forms in the heated portion of turbinate, causing the turbinate to shrink in size.
If a portion of the turbinate is removed, a procedure called a submucosal resection is typically performed. This means that the lining of the turbinate is left intact, but the “stuffing” from the inside of the turbinate is removed. As the turbinate heals, it will be much smaller than before surgery. Sometimes, this resection can be performed with a device called a microdebrider. This device allows the surgeon to remove the “stuffing” through a small opening in the turbinate.



